About
Did you know that vaccines are not equally effective in different regions of the world?
The invention of vaccines for the prevention of infectious diseases has been one of the greatest scientific innovations of all time.
Each year, millions of deaths worldwide are prevented through childhood immunization. [1]
Although the use of vaccines has been a remarkable medical break-through, research findings from across the globe have shown that there are marked variations in vaccine performance across different populations. [2] Suboptimal responses to some vaccines (vaccine hyporesponsiveness) have been observed in some low- and middle-income countries (LMICs) compared to high income countries (HICs). For example, reduced efficacy has been noted for vaccines against malaria [3,4] and rotavirus. [5] In addition, lower vaccine immunogenicity for BCG vaccine [6] as well as the Ebola vaccine [7] has been observed when comparing LMICs with HICs. Even within LMICs, differences in vaccine responses have been observed when comparing people living in rural areas compared to those living in urban areas. [8]
To ensure better performance of vaccines worldwide, there is an urgent need to find the specific factors driving differences in immune responses to vaccines.
Our Mission
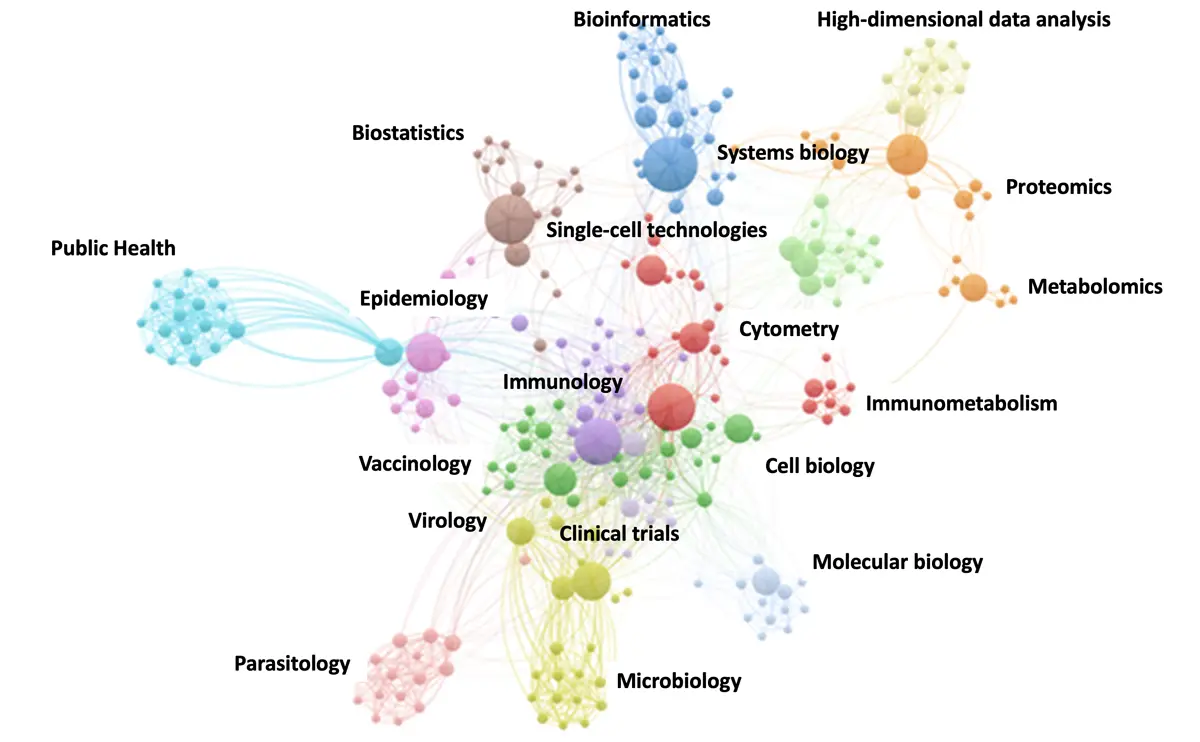
The HypoVax Global Knowledge hub aims to tackle the problem of vaccine hyporesponsiveness by creating a platform that mobilises global researchers working in diverse fields related to vaccines to form a strong network focused on the Global South.
The hub has been initiated through a Spinoza prize awarded to Professor Maria Yazdanbakhsh of Leiden University Medical Center working closely with collaborative partners around the world.
We aim to encourage collaborative teamwork and allow members to share expertise, methodologies, advanced technology platforms as well as data all with the aim of better understanding population-level variations in responses to vaccines.
The hub is committed to promoting diversity in ideas, people and gender as well as addressing the global North-South divide in research while ensuring equal partnerships between researchers from different parts of the world.
Gender imbalances in research still persist and we would address this by supporting and championing women researchers and to facilitate mentorship opportunities.
To ensure maximum utilisation of findings emerging from the knowledge hub, industry partners, technology transfer experts, funders and policymakers will be engaged in co-creative steps.
The hub’s vision is that global researchers work together towards a common goal of finding interventions to reverse vaccine hyporesponsiveness.
references
- Centers for Disease Control and Prevention. Fast Facts on Global Immunization: Centers for Disease Control and Prevention
[cited 2023 02/02/2023]. - Lynn DJ, Benson SC, Lynn MA, Pulendran B. Modulation of immune responses to vaccination by the microbiota: implications and potential mechanisms.
Nat Rev Immunol. 2022;22(1):33-46. Epub 20210517.
PubMed PMID: 34002068; PubMed Central PMCID: PMCPMC8127454.
doi: 10.1038/s41577-021-00554-7. - Mordmüller B, Surat G, Lagler H, Chakravarty S, Ishizuka AS, Lalremruata A, et al. Sterile protection against human malaria by chemoattenuated PfSPZ vaccine.
Nature. 2017;542(7642):445-9. Epub 20170215.
PubMed PMID: 28199305.
doi: 10.1038/nature21060. - Jongo SA, Urbano V, Church LWP, Olotu A, Manock SR, Schindler T, et al. Immunogenicity and Protective Efficacy of Radiation-Attenuated and Chemo-Attenuated PfSPZ Vaccines in Equatoguinean Adults.
Am J Trop Med Hyg. 2021;104(1):283-93. Epub 2020/11/19.
PubMed PMID: 33205741; PubMed Central PMCID: PMCPMC7790068.
doi: 10.4269/ajtmh.20-0435. - Clark A, van Zandvoort K, Flasche S, Sanderson C, Bines J, Tate J, et al. Efficacy of live oral rotavirus vaccines by duration of follow-up: a meta-regression of randomised controlled trials.
Lancet Infect Dis. 2019;19(7):717-27.
Epub 20190606.
PubMed PMID: 31178289; PubMed Central PMCID: PMCPMC6595176.
doi: 10.1016/s1473-3099(19)30126-4. - Lalor MK, Ben-Smith A, Gorak-Stolinska P, Weir RE, Floyd S, Blitz R, et al. Population differences in immune responses to Bacille Calmette-Guérin vaccination in infancy.
J Infect Dis. 2009;199(6):795-800.
PubMed PMID: 19434928; PubMed Central PMCID: PMCPMC3276835.
doi: 10.1086/597069. - Bowyer G, Sharpe H, Venkatraman N, Ndiaye PB, Wade D, Brenner N, et al. Reduced Ebola vaccine responses in CMV+ young adults is associated with expansion of CD57+KLRG1+ T cells.
J Exp Med. 2020;217(7).
PubMed PMID: 32413101; PubMed Central PMCID: PMCPMC7336307.
doi: 10.1084/jem.20200004. - van Riet E, Adegnika AA, Retra K, Vieira R, Tielens AGM, Lell B, et al. Cellular and Humoral Responses to Influenza in Gabonese Children Living in Rural and Semi-Urban Areas.
The Journal of Infectious Diseases. 2007;196(11):1671-8.
doi: 10.1086/522010.